There are days that living with type 1 diabetes is downright difficult. I do something that I’ve done many times before and lo and behold, get a totally different outcome. An outcome that completely sucks and feels horrible for my whole body.
That’s what happened two weeks ago when I got up, ate my normal 30 grams of carbohydrate breakfast, for which when I’m going for a long run, I take zero insulin. I then took my dog Sam for a short walk, got in my car and drove to the run start, which was about 20 minutes from my house. In the car ride to the run start, I ate a packet of UCAN Edge nutrition, which is another 15 grams of long acting carbohydrates.
We started the cold, very, very windy run at 7am. For the first bit of the run my blood sugar was totally fine. Then at a little before 8am my pump made a loud noise. I thought, “Oh no, I’m having low blood sugar, better check.”
I pulled out my phone and opened the t:connect app (the app that tracks my Dexcom continuous glucose monitor (cgm) along with what my Tandem t:slim insulin pump is doing). I almost fell over. I was so surprised.
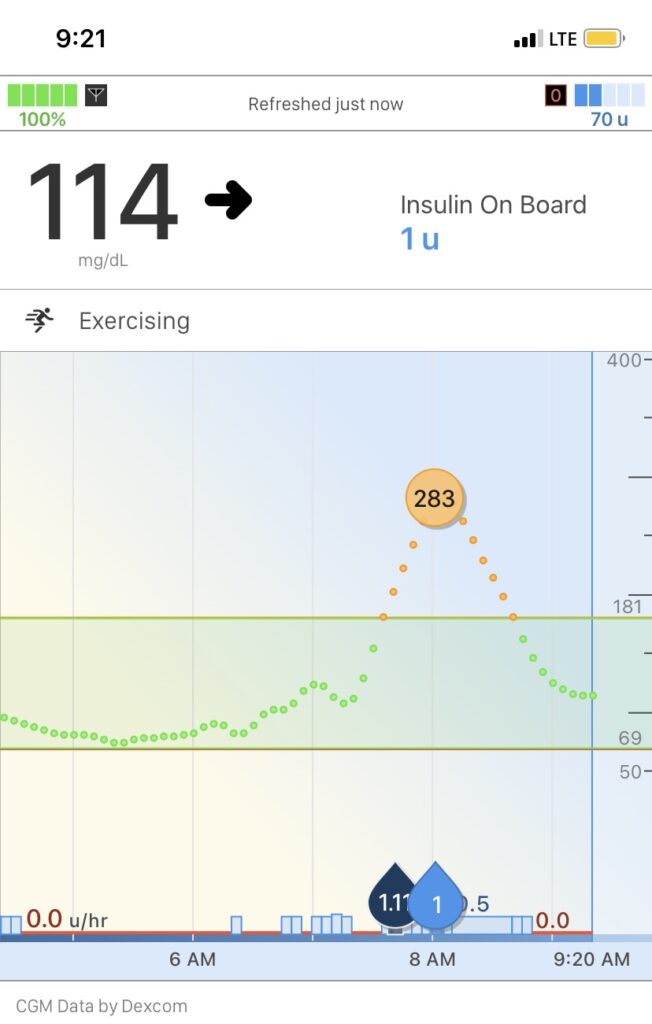
My blood sugar was almost 283 mg/dL, which is what it was at the highest point which it reached at 8am. 283 mg/dL is HIGH. It is NOT GOOD. Normal and ideal blood sugar is between 70 mg/dL and 180 mg/dL.
I had noticed about twenty minutes earlier that I felt extra sluggish and my vision had started to get a tiny bit blurry. I didn’t really think about it, after all, the wind was vicious and it was quite cold and I was attempting to keep pace with the group. I haven’t had a high blood sugar in over two years on the mornings I go out running. I didn’t realize that my sluggishness and slightly blurry vision might be happening because of high blood sugar.
Turns out that was exactly why I felt so awful and couldn’t see very well.
I knew I had to make a choice at that moment. Essentially I had two options to choose from.
Option 1: Immediately stop running and call for someone to pick me up.
If I was a newly diagnosed insulin dependent person with diabetes, this would be the smart option. Blood sugar over 250 mg/dL it is advised to discontinue exercise until the blood sugar has gotten back into a normal range.
The reason is that continued aerobic exercise can be very confusing for the body without enough insulin and the blood sugar could continue to rise. Blood sugar continuing to rise can lead to diabetic ketoacidosis which is when the body creates ketones which is essentially toxic poison for the body.
Option 2: Strategize.
This choice required a few actions.
- Make sure my pump is still connected to my body.
- Take a micro-bolus of insulin.
- Visualize that insulin doing its work of allowing the glucose in my bloodstream to get into my cells.
- Keep running.
I chose Option 2.
Not an easy decision to make due to how awful I felt physically. This is when having lived with type 1 diabetes for more than 40 years comes into play in decision making. Of those 40 years, the past 18 have been spent as an endurance athlete who has had to learn to manage type 1 diabetes on long runs, long bike rides, long swims and on classic cross country skiing outings.
Action Steps to keep running
I started by confirming that my insulin pump was still connected to my body. It was. I had plenty of insulin and battery power in my pump. That was an immediate relief.
Step two was to have the pump calculate how much insulin I needed to lower my blood sugar into the normal range. The pump said I needed a bit more than 2 units of insulin. I took a deep breath and knew that would be WAY too much insulin given how much more running I still was going to do. Aerobic exercise, which long running is for me, in my case, lowers my blood sugar with consistent steadiness.
I noticed that my pump had given me a bolus a bit earlier, that’s the black tear drop you see on the image above. The pump had detected the high blood sugar and had automatically given me 1.11 units of insulin.
The t:slim insulin pump I wear has Control-IQ Technology, which means the Dexcom continuous glucose monitor talks to the pump and makes decisions about how much insulin to give me based on the trending blood sugars. I know from countless finger pricks that the Dexcom is nearly perfect in measuring my blood sugars. As a result, I trust the decisions the Control-IQ makes for me.
I breathed into my decision and decided to give myself an additional 1 unit of insulin, half of what the pump calculated that I needed. That amount is known as a micro-bolus. A bolus is the insulin you give yourself to cover a high blood sugar or to cover the carbohydrates you are eating. A micro-bolus is a smaller amount of insulin given to nudge the blood sugar down, but not an amount that could cause a rapid decrease in blood sugar. The insulin in combination with my continued running effort would get my blood sugar back to the normal range.
The real challenge began
I didn’t tell any of the people I was running with that I was navigating a slightly dangerous high blood sugar. I didn’t want to have to explain as I was running as I felt physically awful about what was happening in my body. I simply kept running. I did drink all the water in my Flipbelt water bottle. I knew we had another water stop ahead as Run Minnesota, the club I am a part of, provides water stops on our long run Saturdays. Water helps the kidneys flush the sugar out of the blood and out the body (yes, I’m talking about peeing.)
Alone time for mantra recitation
At one point, I purposefully dropped back on the hill we were running. I did that so I would have a few minutes alone. I needed the alone time so I could 100% focus my energy and on what was happening in my body. I breathed deeply and began my mantra recitation.
“Body, feel the insulin. The insulin is working. Insulin allows the glucose into the cells. The cells need energy. It’s coming in, via the insulin key. Trust. Insulin, I see you working. I see you helping me. I believe you are helping me.” This is what I repeated over and over in varying forms. Essentially, I kept reminding myself and seeing the insulin doing its job.
It wasn’t immediate. It took nearly an hour, during which time I was continuously running, to get back into normal blood sugar range. I had to restrict how often I would look at my phone to see what my blood sugar was doing. Instead, I kept up with my mantras and my visualization.
I joined back up with the group and joined in friendly banter as we chatted as we ran. This was a particularly challenging route, as we crossed three long bridges where the wind kicked up as we crossed the Mississippi River twice. All the talk and the wind and the bridges gave me something besides my high blood sugar to think about and do while I gave the insulin time to work.
Made it back to the run end
Finally we got back to our cars. Originally the plan was to run 8 miles. We had the option to do a short out and back to add on the additional mile. No way. I was ready to head home. By the end of the run, my blood sugar was completely in the normal range and besides being worn out, I felt pretty good.
I drove home. Right after my shower and a tasty protein carbohydrate snack, I studied my Dexcom tracing on the t:connect app. I wanted to figure out why this high had happened.

Living with diabetes is a science experiment that requires investigation
If you study the photo of my blood sugar tracing above, you will notice along the bottom at 6AM and more than an hour before 6AM there is a red line along the bottom. At the start of the red line it says 0.0 u/hr. That means that starting at about 4:30AM my pump detected that my blood sugar was getting low and it shut off my basal insulin.
Basal insulin shut off
Basal insulin is the background insulin my body needs to keep my blood sugar in a normal range. My body makes absolutely zero insulin, so there is nothing my body can call on in terms of insulin. Yes, I’ve been tested, as some people with type 1 and most everyone with type 2 have some background insulin. Not me, zero background insulin is made by my body.
No insulin means high blood sugar
The morning of this run, I did not notice that I had no background insulin when I chose to eat my normal 30 grams of carb breakfast and 15 grams of carb UCAN packet. As my body digested the breakfast and the UCAN, I had zero insulin to help those carbs get into my working cells. The running I was doing was not enough to get the glucose from my bloodstream into my cells. My body reacted and up, up, up went the glucose in my blood.
Once the pump gave me 1.11 units and I supplemented that with 1 more unit, right away my body could get the glucose from my bloodstream into my cells.
What to do next time
Studying what happened, made me realize that going forward, I need to study the cgm tracing more carefully before deciding whether or not I would take insulin for the breakfast and UCAN I would eat.
That’s exactly what I did the next week. You’ll see in the photo below that my pump did not shut off for as long as it had the week before, but it had shut off for a little while. As a result, I took a micro-bolus for the breakfast food I ate. It worked. While I was running, my pump did shut off the basal, but that was okay, because I was running and I wasn’t consuming many carbohydrates.
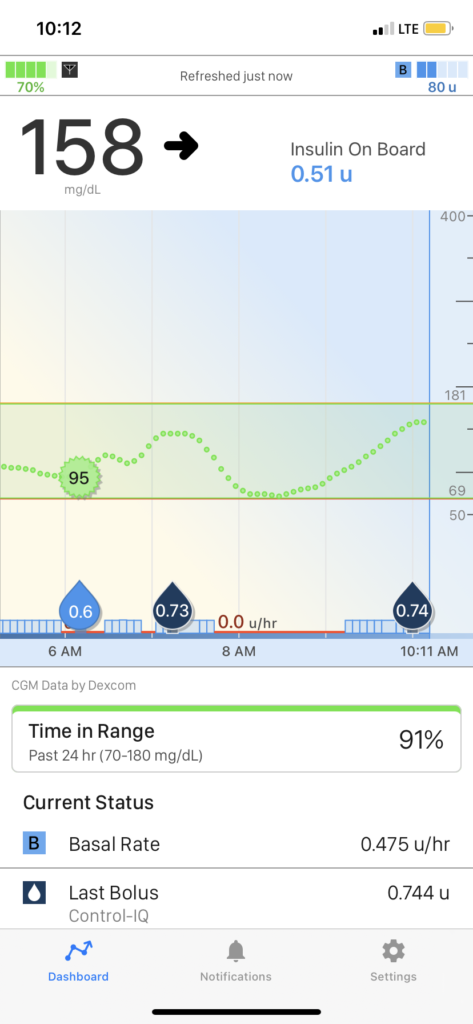
There you have it. Insulin dependent diabetes keeps those of us who deal with this disease on our toes, alert and constantly navigating. This description of what happened to me a few weeks ago gives those of you reading this a birds eye view into what insulin dependent diabetes is like. I rarely talk about it. I just deal with it.
I appreciate that you took a moment to read what I wrote today. I hope it gave you a glimpse into my world.
If you’d like to support my Tour de Cure Minnesota bike ride that I will do with the American Diabetes Association on June 4, 2022, it would mean the world to me.
Are you on my email list yet? If not, please sign up today! That way we can stay connected!
You are such an inspiration Mari! To be this in-tune with your body and what it needs and how to get it there, is a gift!
Thank you Marie for your very kind words!! You’ve been out there with me at various athletic events/trainings when things have gone diabetes haywire, I have appreciated your support and kindness!! That makes SUCH a big difference!!
Wow! Amazing. Now I see why so many people don’t persist in being active when they run into trouble like this and don’t have your determination and ability to think under difficult circumstances. Thank you for sharing these details. I know they will help others who want to navigate complicated situations.
Thanks for your kind words Linda. Insulin dependent diabetes is indeed a challenge that calls up my determination and challenges me to keep calm under difficult circumstances. Keeps me on my toes!